Science is on the verge of discovering at incredible fast steps the astounding connection between gut health and overall health.
Terms as the brain-gut axis and the second brain referring to the gut are common now in the scientific world with leading investigation institutions working in the field. Amazing findings have been made, like the fact that the same neurotransmitters that are produced in the brain, like serotonin, dopamine, and endorphins are also produced in high levels in the gut. Short-chain fatty acids, with vital roles in health, are also produced by healthy microbiota in our guts as a byproduct of feeding it with the right food, as the soluble fiber contained in the yacon root syrup.

Medical science over the years has evolved; year after year advances in medicine develop new ways of diagnosis, treatments and better health care practices overall. No doctor in the world is able to know all the enormous amounts of knowledge that medicine formulates every day, so specializing allows doctors and health care professionals to focus on a particular area of knowledge, to learn it thoroughly and become an expert in that area.
One area of medicine, the area of psychiatry, focuses on mental problems examined from two main areas:
- Childhood influences
- Experiences and genetics
Until modern psychiatry started to link psychiatric conditions by looking at the patient's digestive system in this post we ́ll talk about how your diet can influence the way you feel. Let's find out why and how.
THE WHY
Recent studies [1] have found that the majority of psychiatric patients suffer or have suffered in the past from digestive problems, gut-related alterations that are largely ignored by doctors. The gut-brain connection is a topic which traditional medicine does not want to acknowledge or does not want to understand, giving instead millions of pharmaceutical prescriptions involving antidepressants, sleeping pills and other powerful drugs that patients have to put into their digestive system, dealing mostly with symptoms but not with causes. However, in the last few years, stronger and stronger scientific investigation and evidence are demonstrating the intricate, powerful connection and interaction between our gut, our brain, and our overall health.

Take for example alcohol consumption and the effect it has on our brain, the metabolism of ethanol (alcohol) have profound effects on our way of feeling and thinking, so when it comes to drugs they are no exception, drugs metabolism have undesired side effects that are no stranger to the gut, leaving our gut in a state of dysbiosis, a clinical term for a negative microbiota imbalance.

In a previous post, we talked about microbiota, gut health and how fiber, -especially soluble fiber like the one in the yacon root- in the diet can influence good and bad bacteria populations. Today we are going to dive a little bit deeper about how it affects the brain.
Anatomically, microbiota resides in various tissues inside our bodies [2], nevertheless, the gut is the most important one. Hosting it by the trillions, it is the headquarter of operation and therefore in bioactivity, affecting countless functions and processes in our bodies. It changes every time depending on what we eat or drink, be it food or medicines and changes can be for good or bad. As you can guess constant ingestion of drugs can change our gut microbiome for bad, leaving us with a very low number of good bacteria that is a synonym of Dysbiosis is the clinical term for a negative microbiota balance, where pathogen gut bacteria outnumber the beneficial ones.
THE HOW
A state of dysbiosis leaves our gut unprotected, becoming a major source of toxicity, toxicity happens because bad bacteria produce substances called metabolites, not all metabolites are bad, but the ones produced by bad bacteria are toxic as they build up to a certain point; -toxic metabolites-.
These toxic metabolites are absorbed through the blood and taken up by the brain. When these toxins get there they become neurotoxins, neurotoxins are described as destructive to nerve tissue [3], damaging or interfering with neuron connection that can adversely alter brain function and therefore set the tone for the onset of mental illness.
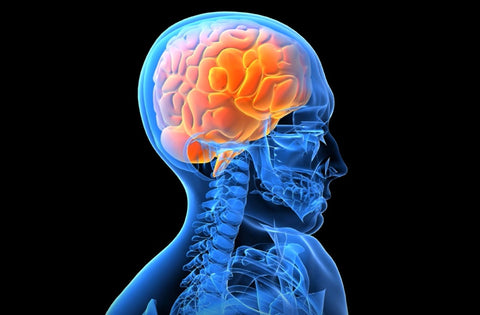
EAT GOOD, FEEL GOOD
Before the era of pharmaceuticals, the psychiatrist diagnosed patients not only with psychiatric problems but also with undernourishment. Research [4] [5] proves the deficiencies in Vitamin B, Vitamin C and other minerals like magnesium and zinc in several patients diagnosed with Depression and Schizophrenia.
Taking that into consideration, from a nutritional point of view, a state of dysbiosis is almost certain to trigger deficiencies in many micronutrients, as bad bacteria can alter the metabolism and proper absorption of several nutrients.
Even more, once, a french psychiatrist Phillipe Pinel almost 200 years ago wrote, “the primary seat of insanity generally is in the region of the stomach and intestines.'' An incredible forecast of what solid scientific research is asserting now.

Gut health and the resulting nutritional status are being taken into consideration more and more in modern medicine.
Today's topic is a very relevant one, a topic that brings new insights not only to psychiatrists, nutritionists, biologists, medicine professionals in general to work together in current diagnosed patients to come up with better treatments, but also to other populations out there to start caring more about the value of good nutrition and rely less on drugs.
At Wholefort we truly believe in the power of food to reach your optimal health Thus as part of our quinoa breakfast cereals, we have formulated one with yacon root syrup. Yacon root syrup is an outstanding source of soluble fiber proven to nourish and sustain only the good bacteria in our guts. In each serving size of our quinoa cereal with yacon, you will get the recommended daily dose of soluble fiber.
REFERENCES - Written by Antonio Reyes RDN
-
Baranowski A, Kondrashina E. Colonic dysbacteriosis and dysbiosis. Saint Petersburg Press. 2002
-
Gibson GR, Roberfroid MB (1999). Colonic Microbiota, Nutrition, and Health. Kluwer Academic Publishers, Dodrecht.
-
Rogers S. 1990. Tired or toxic? A blueprint for health. Prestige Publishers.
-
Baruk H. 1978. Psychoses of digestive origins. Biological Basis of Schizophrenia. Lancaster MTP Press.
-
Wittenborn JR. Niacin in the long term treatment of schizophrenia. Arch Gen Psychiatry, Vol 28, 1973, pp. 308-15.


